

(Make sure your sound is turned on. Please wait up to 10 seconds for the video to load)


(Make sure your sound is turned on. Please wait up to 10 seconds for the video to load)
The 7 Steps to Health is the ONLY doctor approved and scientifically verified system to give you the secrets to reverse your diabetes and lose weight PERMANENTLY IN 2019 without drugs, pills, more exercise, or feeling like you are on a "diet" at all…
Regain your blood sugar, lower and even completely eliminate your drug dosages, and get cleared as "healthy" by your family doctor!
For everyone it's different…
For some of you, you’re struggling with diabetes, and you've tried everything (might be in your family history, or you're suffering for decades).
For others, you are fed up with diabetes drugs, pricking your finger, or constantly watching what you eat.
You might not know where to start, you’re struck, lost and confused about what to do.
Maybe you're looking for something to help you finally get clarity about reversing this condition for good, losing some (or a lot) of extra weight, and just be happy! (without feeling deprived, or "feeling like you’re on a diet" at all)
Are you struggling to keep your blood sugar in the healthy ranges and you want to get results fast? (From 270 to 90 in record time)
Have you suffered with diabetes or just been diagnosed with pre-diabetes, and are scared about your future?
Are you taking diabetes medication and looking at you blood glucose daily? (you can have your doctor take you off your medcation completely within just weeks)
Want to lose a little or a LOT of unwanted fat from your stomach, thighs, or butt, and have NO IDEA where to start?
Are you convinced that you need a blueprint, but not sure where or how to start? (without depriving yourself, counting calories, or relying on deadly drugs or medications)
Want to finally transform your body and your health and be happy each and every day!? (without actually "dieting" or taking out the good things in life)
You will get immediate access to the 7 Steps to Health manuals showing you the shockingly simple "glucose normalizer" system with the recipes and powerful compounds to turn your body into a "Diabetes Destroying Machine"…
The "Secret Blood Sugar Remedies" that have been used for thousands of years by indigenous populations to prevent the dreaded "Blood Sugar Spike" and the simple food that is probably in your fridge right now that is killing your pancreas and makes it virtually impossible to have healthy sugar levels…
Turn your body into a "blood sugar-destroying-machine" by elevating the levels of this "Master Insulin Hormone" by an astonishing 2000% to burn away the unwanted fat while you sleep at night (without taking a single drug or pill, completely naturally)…
The "Fat Melt" oil that forces your body to use fat cells as energy gobbling up the excess from your stomach and thighs (just a few teaspoons can supercharge your fat loss)…
How to "Feed" your brain and libido with this secret yellow compound that raises metabolic rate, helps remove abdominal fat, boosts muscle growth, reduces resistance to insulin, strengthens the immune system and lowers food allergy reactions, has all 37 vitamins, minerals, and amino acids…
The "Time Machine" principle and how you can turn back the clock even if you are in your 40s or 50s to regain glowing skin, massive improvements in energy levels, and feel like you did in your teenage years (it's all due to your mitochondria, and a peculiar pH blood principle, its so simple you will be astonished at the results)…

Learn about the deadly compounds in your everyday foods that destroy your feel-good hormones leading to terrible "Don’t Touch Me" moods, and the simple dietary change that can eliminate them leading to increased happiness levels within just days.
Learn about a few types of "Fat destroying" nuts, and how eating just a tiny bit once a day helps to decrease fat cell count leading to supercharged weight loss (PS. They're really tasty, you’re gonna love them)…
Lean about the "Hunger Switch" and this simple routine that can turn off your "Fat Gain Impulse" inside of your body leading to less food in, and more fat burned (Its so easy, and doesn’t require anything, you can actually do this today).
Discover how these simple sprouts have been reported to contain 10 or more times as much sulforaphane, a cancer protective substance than broccoli. In a Swedish study, it was reported that eating 3 or more servings a week of these delicious foods significantly reduced the risk of stomach cancer, the fourth most frequent cancer in the world.
Learn about this sweet herb you can use instead of sugar which lowers elevated blood pressure (hypertension), acts a digestive aid that also reduces gas and stomach acidity, and helps "melt fat" right off (The herb acts as general tonic which increases energy levels and mental acuity too).
Discover the TRUE REASON why you ALWAYS seem to get SICKER and LESS HEALTHY after taking drug after drug… pricking your finger to no end… following those "diets" year after year, and learn about all these groundbreaking methods, which are as simple as "counting your ABC's" but can forever eliminate your frustration or deadly symptoms, and finally give you the famous "diabetes reversal" hallelujah!


Then you absolutely NEED to start the challenge and read this book as soon as possible. You can actually flip through the pages day-by-day, and SEE the “big picture” of your plan laid out right in front of you! You can HOLD it in your hands…
Learn about the simple foods found in any grocery store that:
Some people find out the hard way, by relying on drugs and medication to try to beat their disease (but you know that using pharmaceutical drugs has never brought you the results you desire). The "lie you have been told is that you HAVE to take diabetes medication for the rest of your life… before you suffer more serious complications, like lose your vision, have to be amputated, or even die from diabetes…
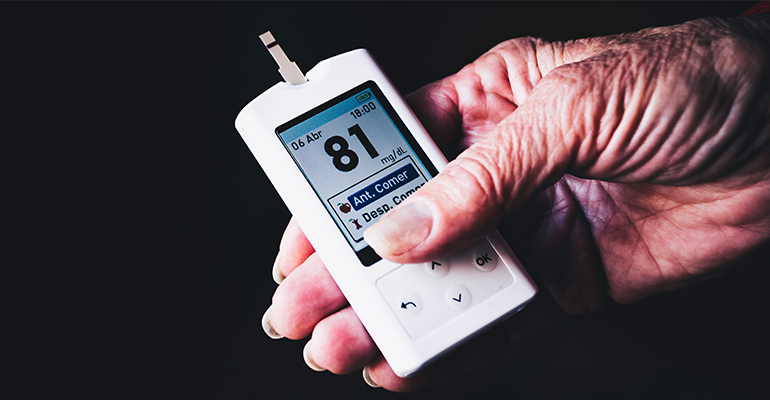
This is scary! And it's something I DO NOT want for you…
With the revolutionary 7 Steps to Health program, you could easily start the "backwards" process to target each symptom, each cell, and your pancreas to start the process of natural healing your condition…
I don’t want you to waste decades trying things that don’t work. Save yourself the headache and the heartache, skip the things that don’t work, and do what is guaranteed to make you lose 10, 20, 50 pounds of unwanted fat, have your doctor take you off your medication, and pronounce you "diabetes free"! (Get compliments from people and looks AMAZING on your next vacation or day at the park or beach)

Our 350,000 clients in over 40 countries have already seen and felt the difference, and those who follow our SUPER SIMPLE program see results very quickly, and their doctors took them off their medication and declared them "healthy" in mere months…
And if you have some extra nagging weight, you can start losing 5, 10, 20, or 50 pounds of extra weight safely and easily.
You will have the knowledge to transform your body and your health at your fingertips.

When you join the "7 Steps to Health Challenge" today we are going to send you a kit with the 300 page '7 Steps to Health' book, the 60 days of full coaching and support at your fingertips, the Deliciously Simple Recipe book, Exercises, Simple Start Guide, 5 Bonus books, and more!
Let me show you a glimpse of a few of the cool things that come in your program kit!

(37$ value)
 Start the 7 Steps To Health challenge now!
Start the 7 Steps To Health challenge now!

What if you had the KEYS to unlock the healing and turbocharge the glucose normalizing capacity of your body?
The exact blueprint to get from where you are to where you want to be?
The most powerful tools to propel you into a life of health, vitality, and perfect weight!?
It would be an invaluable manual wouldn’t you agree? Well, it is here, and it is only minutes away from you reading the first few pages.
Combined is the absolute best foundational and advanced knowledge for those who have tried everything but want to start making real change in their diabetes starting today (your doctor is going to be shocked, and your friends will beg you to know your secret).
How to achieve 100% faster diabetes reversal (including all the symptoms, with a "NO BS" science and physiology approach into the most groundbreaking research NOW, and actual get results starting on DAY 1).
The medical and drug lies that are keeping you sick and unhealthy (the pharmaceutical industry would rather you NOT know these).
The groundbreaking studies and compounds which you can start using TODAY to get healthy (your doctor will take you off your medication and declare you in perfect "health").
And a lot more… The 7 Steps to Health program teaches people how to heal their pancreas, normalize blood sugar, blood pressure, and achieve their weight and health goals in less time, with less work, as proven by renowned Institutes and oldest indigenous populations without any diabetes…
($497 value)
 Start the 7 Steps To Health challenge now!
Start the 7 Steps To Health challenge now!
Everyone who achieved incredible results in their healing, perfect blood sugar, perfect weight and health had three things:
1. A strong goal
2. A strong support network
3. A blueprint for success.
For 60 days and beyond you get access to our support and coaching lines, to eliminate the roadblocks, the frustration, and the hassle.
Our coaches are going to answer any diabetes, health, or weight loss question you might have and make this process easier, clearer, and smoother. We will practically guide you by the hand to get you the diabetes and health results you desire (with our help they will come much faster than with anything you migh have tried before, because everything is proven to work).
Frustration and confusion is the enemy of lightning fast results.
This is why we have create a Simple Start Guide and Level System, which will give you a quick understanding of the whole challenge so you can get started immediately, literally within 2 minutes from now…
Life is about being diabetes free, without any ugly extra weight, and having plenty of energy to look good and feel good, this is why it is absolutely critical to get actionable steps right from the start…
This guide is absolutely vital if you want "complete control" over your blood sugar and to put your weight loss on TURBO, so get clear, get focused, and know EXACTLY how to reach your dream body and health.

($37 value)
 Start the 7 Steps To Health challenge now!
Start the 7 Steps To Health challenge now!($37 value)
 Start the 7 Steps To Health challenge now!
Start the 7 Steps To Health challenge now!

Let's be honest, living with diabetes is hard, and its even harder when you have to be counting calories, eating tiny meals, or putting yourself on a 18th century prison diet made up of wool, woodchips, and water…
In reality, dieting is bad for you, it's destroys your health, and it is terrible for keeping your fat loss for decades to come... (plus, nobody has time for it in their busy lives).
Your body is an incredibly fine-tuned machine, you can't just eat bland diabetes food and expect to live a happy life!
The "diabetes destroying" compounds that you will discover are incredibly simple, and they have a MASSIVE effect on healing your blood sugar, and diabetes symptoms (just a few teaspoons a day can start the healing process immediately).
In reality, what you eat has the biggest effect on your heath than virtually anything else in life. Having delicious foods by your side that nourish you, feed you, heal you, and help you lose weight is CRITICAL in getting your diabetes symptoms under control getting that unwanted weight off faster and sooner.

Since we want you to have the absolute best health package available today, we're throwing in 5 bonus guides on some of the most important health issues that you absolutely need to incorporate for even faster diabetes reversing results.
Learn how to put a stop on deadly free radicals and inflammatory acidosis that makes diabetes worse, wreaks havoc by damaging DNA, corroding cell membranes and killing cells outright.
Dr. Denham Harman, MD, Ph.D. University of Nebraska College of Medicine states: "The relationship between aging and disease involving free radical reactions seems to be a direct one antioxidant supplements will increase the healthy, active life span by 5-10 or more years".
Discover the "sleep pattern" techniques used by some of the most prominent athletes and trainers to heal, restore, and rejuvenate.
Did you know that exposure to even dim light at night, such as a glowing TV screen could prompt changes in your brain that lead to mood disorders, up to and including depression?
There are 3 incredibly simple things which most people simply don’t know that can turn their sleep into a powerhouse rejuvenating process, allowing you to fall asleep faster, sleep less, and feel more refreshed than ever.
Learn how to lose more weight, have no more day time fatigue, improve your blood pressure and much more, simply by drinking the right water, in the right amounts, at the right time.
And learn about all the harmful toxins, petrochemicals and immuno-suppressants floating in your tap water and how to remove them.
These guides will add a massive impact on your diabetes health and increased body rejuvenation. Your health journey is not complete without them, so take advantage of this bonus offer!
($162 value)
 Start the 7 Steps To Health challenge now!
Start the 7 Steps To Health challenge now!

A method that is proven, doctor verified, and has decades of research behind it…
Even deadly conditions like heart disease, diabetes, or other serious disease symptoms can be stopped…
Normalize your cholesterol, blood pressure, and blood sugar levels…
Slow the aging process…
Lose that extra weight faster and easier…
Destroy scary degenerative processes within the body…
Remove toxicity buildup in the kidneys, liver, pancreas…
Renew the smooth lining within the heart arteries leading to a healthy heart…
Rebuild blood vessels and tissues…
Create perfect health and vitality…
And do it in record time, do It safely, do it in a way that is both fun and challenging, and one that does not prevent you from enjoying life…
If you don’t have these conditions, imagine the amount of people you can help with this knowledge. Your family, friends, relatives, will be thankful beyond belief, you can be that beacon of hope for them.
What if you had the KEYS to unlock the healing capacity of your body?
The exact blueprint to get from where you are to where you want to be?

The most powerful tools to propel you into a life of health, without diabetes, and perfect weight!?
It would be an invaluable manual wouldn’t you agree? Well, it is here, and you are only minutes away from you reading the first few pages.
You can definitely agree this is a bargain basement price for your whole body transformation…
And if someone offered you a $800 dollar discount on something, you would probably rush to get it before anyone else tried to take it away…
To claim your discount and take advantage of this incredible offer, all you have to do is click the big button below, right now…
We have never offered these programs for such a discount, but we are doing it for your benefit…
For the benefit of hundreds of thousands around the world who have already taken action and are reversing their diabetes, throwing away their medication, losing pounds of fat starting on day 1, and finally living their life on their terms…
But you have to act fast, this deal could be taken down tomorrow and double in price…
So I can't guarantee if you come back even 30 minutes from now that the price will be the same…
So click the order button below and get started immediately…

Here’s how it works:
1
Just enroll in “7 Steps to Health” program right now…
2
USE the material… (It’s so easy to use and as close to “Done For You” as humanly possible).
3
See for yourself how EASY getting PERFECT blood sugar, firm, FLAT belly and watching the pounds FALL off your body can actually be…
If you don’t think “7 Steps to Health” is worth at least double what you’re paying today, just contact our customer service at support@theitmc.com any time in the next 60 days…
And you’ll get every dime back as fast as we can (usually the same day)…
We have so few people asking for their money back, that we truly know this is the best total health program in the world…
If you are asking yourself why we are so generous with this program and the price…
It really comes down to the fact that the more people experience these breakthroughs, the better the world will be as a whole…
This is our "evil" ulterior motive - for you to change your life and make the world a better place…
We want people to be healthy, and not dependent on drugs or pills, or being a slave to their condition…
After all, our children will be living on this planet long after we are gone, and we want to leave them the world in a better shape than when wer were here…

In fact, this is the reason we are willing to give the entire program to you for just 37$, since we are so excited about this idea of a better future for you and a better world for us!
Our philosophy is simple. We want to help you change your life in a meaningful way, then we all win as a human race…
Does that sound more than fair? :)
We want you to experience a new life, and a new body YOU LOVE looking in the mirror at…
To get compliments from your friends, family, and being full of enthusiasm…
To be symptom free, declared "healthy" by your doctor, who is going to be shocked at your transformation…
To toss out your medication, and forever end the need to test your blood sugar…
To lose that ugly fat, and finally be PROUD to look in the mirror…
Now it's your turn, start your transformation today!
 And all you have to do is click the order button now, and forget that you've ever had diabetes…
And all you have to do is click the order button now, and forget that you've ever had diabetes…
Price goes up at midnight!
|
Privacy|
Terms & Conditions|
AffiliatesEvery inspiring weight loss story you see on this page is a real person who got verified results using the exact methods from the 7 Steps To Health manual. They followed the system to the letter to get these amazing results. However, although we work hard to ensure it's easy to do so, the typical user of virtually all education products treats them in much the same way they treat a book. The vast majority read or skim through it once, then do not implement the program or take any recommended action. If you want results like the folks you see on this page you will need to follow the exact diet and supplement strategies outlined in our system. Therefore, reports of specific fat loss, muscle gain, abdominal definition, or any positive results of any kind should be understood as the exception rather than the rule.
Have Any Questions? We're Happy to Assist!
For product support, please contact us HERE





